This article first appeared in The Edge Malaysia Weekly on August 22, 2022 - August 28, 2022
Malaysia’s public healthcare system has been ranked among the best in the region, according to some surveys. Thanks to government funding, public healthcare services are accessible and affordable.
However, population growth and the increase in demand for healthcare services have begun to put a strain on the healthcare system.
This was especially evident during the pandemic, when resources in Malaysian hospitals were stretched thin. Pressed by taxing workloads and no opportunity for career advancement, contract doctors held a strike last year.
Evidently, a reform in the healthcare system is needed. The urgency increases with the expected impact climate change will have on health.
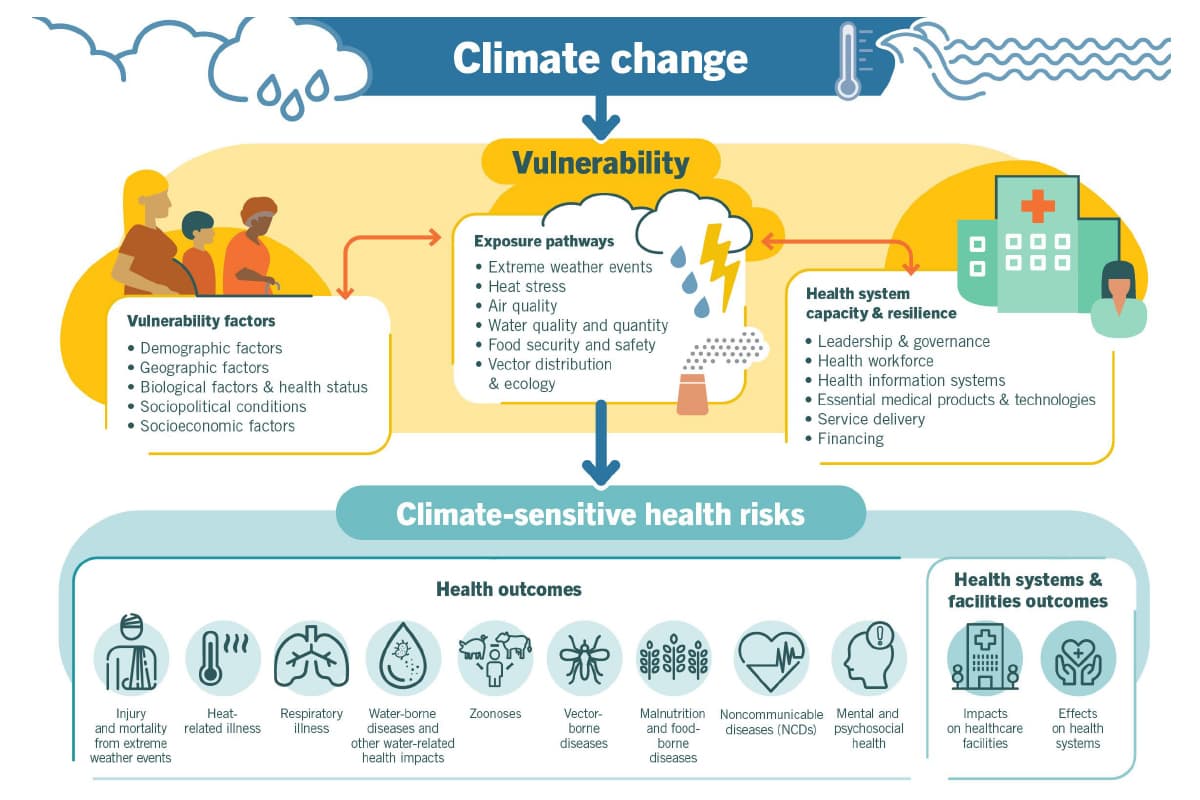
Higher average temperatures, more frequent rainfall and flooding will result in more zoonoses and vector-borne diseases, according to the World Health Organization (WHO). It calls climate change the biggest health threat facing humanity.
“Climate change and rapid urbanisation, in terms of land development and forest clearing, increase temperatures and rainfall. [They] also accelerate the development and production of the vectors,” says Dr Nasrin Agha Mohammadi, associate professor of environmental and public health at the Faculty of Medicine, University Malaya.
Zoonoses are infectious diseases, like the coronavirus, that jump from a non-human animal to humans. Vector-borne diseases are caused by parasites, viruses and bacteria that are carried by organisms like mosquitoes. Examples are dengue and malaria.
Hotter temperatures globally expand the range that vectors can travel, thus increasing the spread of diseases. Water and food-borne diseases like respiratory infections, leptospirosis, diarrhoea and cholera are common during and after flooding events, according to the Ministry of Health.
Malaysia has recorded 20,195 cumulative reported dengue cases so far in the first half of 2022, which is an increase of 65.7% from 2021 for the same period, according to WHO.
While Malaysia and Southeast Asia are less at risk of severe droughts compared with flooding, the incidences of drought in certain geographies are still expected to increase, according to the World Bank’s Climate Risk Country Profile: Malaysia.
“Dry weather and droughts will cause extremely debilitating haze and respiratory problems. In turn, we will see increased hospital admissions for asthma, other respiratory diseases and eye diseases due to inflammation triggered by the particles in haze. Allergy cases will also be on the rise,” says Hakim Hamzah, secretary-general of the Malaysian Red Crescent Society.
Between 2030 and 2050, WHO estimates climate change to cause about 250,000 additional deaths per year from malnutrition, malaria, diarrhoea and heat stress. The direct damage costs to health are expected to be between US$2 billion and US$4 billion a year by 2030.
Another less direct health impact is the stress on one’s body and mental health due to urban overheating by climate change, observes Nasrin.
Humidity and high temperatures contribute to discomfort and heat stress. This causes mental distress, since the body is constantly trying to adapt to its surroundings.
WHO has highlighted that while nobody can escape the impact of climate change, the ones who are most affected by it are those who contributed the least to the crisis.
The disadvantaged and vulnerable populations from developing countries are at risk of sinking deeper into poverty as they struggle to cope with natural disasters and increasing health risks. It will also affect their access to food supply.
“While the general population in Malaysia is being impacted by the climate crisis, the B40 is the most affected compared with the M40 and T20, since they have no other alternatives to get their [food] supplies,” says Hakim.
“Climate change has reduced water quality [and] due to the scarcity of water, food supplies will be disrupted. [Owing to this], food prices will skyrocket and make it difficult for the ordinary person [to access food].”
Building capacity to handle challenges
But these health risks can be managed if proper action is taken ahead of time. For instance, to prevent the spread of dengue, the community must take precautionary measures and practise good waste management. This can be done without waiting for policymakers to make a move, says Nasrin.
“It is important to involve city planners, non-governmental organisations and the community in the area and prepare them in terms of running roadshows, workshops and talks. This is where we have to start instead of just enforcing laws.”
Policymakers, meanwhile, should work with experts from various fields to predict future outbreaks and prepare accordingly.
“Historical data plays a pivotal role in predicting patterns and [informing decisions on] intervention to prevent infectious diseases. By looking at climate data, [experts] can develop early warning systems and improve the forecast of rainfall, as infectious diseases can arise from floods,” says Nasrin.
There must be collaboration with international organisations, adds Hakim, since climate change is a global challenge.
“Collaboration and cooperation between the Malaysian authorities and international players are needed to prepare for the worst and address climate change. We need a wholesome approach by nations across the globe,” he says.
Additionally, it is crucial for Malaysia to nurture experts in the medical and scientific fields who can handle these crises. They must come from different fields and be able to propose feasible solutions to mitigate or address climate change-related challenges, says Nasrin. Access to data is also an important prerequisite.
“Having good data is important. Data accessibility is an issue in Malaysia. By having health and historical environment data, the science behind these disasters will be explored. The trends and correlation of the data will help us manage any predictable disasters with proper standard operating procedure (SOP). I think our authorities must allocate some of this facility for scientists to look into,” she adds.
Save by subscribing to us for your print and/or digital copy.
P/S: The Edge is also available on Apple's AppStore and Androids' Google Play.

